This cool treatment is covered
Cold therapy is an exciting new treatment for people looking to improve their wellness or relieve pain. The Iovera treatment provides pain relief without relying on potentially addictive prescription drugs. Medicare can cover the Iovera treatment if you meet the eligibility requirements. A physician that accepts assignment must deem the treatment medically necessary to receive coverage.
Speak with a Medicare Advocate
What is the Iovera Treatment?
The Iovera treatment is an innovative procedure used to treat muscle spasms and pain. It uses a specialized device that delivers cold temperatures through the skin, targeting precise areas with extreme accuracy and providing temporary relief of targeted muscles. The Iovera treatment is non-invasive, safe and effective. It can be used on multiple body parts, including shoulders, neck, wrists, elbows and more. Many knee replacement recipients use the Iovera treatment for pain relief.
Medicare coverage of the Iovera Treatment
To be eligible for Medicare coverage of the Iovera Treatment, you must meet certain criteria. Your doctor must deem the treatment medically necessary and acceptable according to Medicare's standards. Also, your physician must accept assignment from Medicare in order for the treatment to be covered. If you are a knee replacement recipient, it is likely that you will qualify for coverage as the treatment is often used for pain relief.
The cost of the Iovera treatment will vary depending on your Medicare plan and whether or not you get approval. According to our Medicare experts, the best way to lower your out-of-pocket costs is to sign up for Medicare Supplement Plan G.
How do I find out if I am eligible for Medicare coverage of the Iovera Treatment?
If you think you may be eligible to receive Medicare coverage for the Iovera Treatment, speak with your doctor, who can advise you further. They will be able to assess your condition and determine whether or not the treatment is medically necessary. Your doctor can also help you find out if they accept assignment from Medicare in order for the treatment to be covered.
Potential risks associated with the Iovera treatment and what to do if something goes wrong
Though the Iovera treatment is generally considered safe, there are certain risks associated with the procedure. These include pain, redness and swelling at the injection site, as well as headache and dizziness. If you experience any of these symptoms after receiving the Iovera Treatment, contact your doctor immediately for further advice. You should also confirm with your doctor that you are a good candidate for the Iovera treatment, as this treatment is not for everyone.
Tips on selecting a provider for the Iovera treatment
When selecting a provider to administer the Iovera Treatment, it is important to look for one that has experience in giving the procedure. Ask your doctor for recommendations and do some research on the provider’s background. Ensure they are licensed and insured and have sufficient experience administering the procedure. You should also ensure that they accept assignment from Medicare for the treatment to be covered.
Questions you should ask your doctor before getting an Iovera treatment
Before getting an Iovera treatment, you should ask your doctor the following questions:
What are the potential risks associated with the procedure?
How long will the effects of the treatment last?
Is this a covered service under my Medicare plan?
Are there any other treatments that may be more appropriate for my condition?
What are the possible side effects of the treatment?
How long is the recovery period after a session of Iovera Treatment?
Are there any lifestyle changes I should make to ensure the best results?
Does your practice accept assignment from Medicare?
By asking these questions, you can help ensure that the Iovera treatment is right for you and your condition.
Conclusion
If you are a knee replacement recipient and think this might be the right choice for you, make sure to speak with your doctor about it. They can assess your condition, determine whether or not the treatment is medically necessary, and help you find out if Medicare covers it. This content is for informational purposes only. Don't hesitate to reach out to Fair Square
Recommended Articles

Medicare Guaranteed Issue Rights by State
Feb 10, 2023
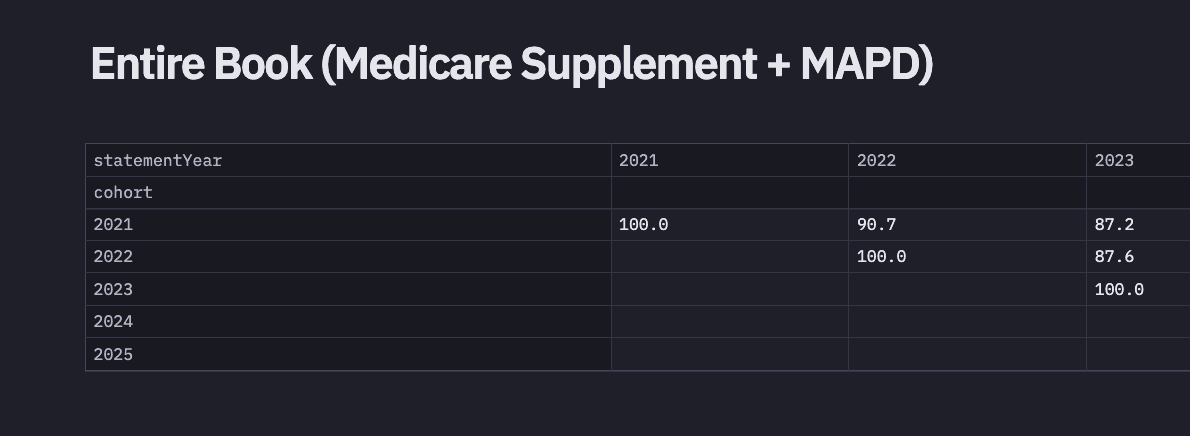
2024 Fair Square Client Retention and Satisfaction Report
Mar 4, 2025
Does Medicare Cover SI Joint Fusion?
Nov 28, 2022
Is Balloon Sinuplasty Covered by Medicare?
Dec 1, 2022

Medicare Advantage MSA Plans
May 17, 2023

14 Best Ways to Stay Active in Charlotte
Mar 9, 2023

14 Best Ways for Seniors to Stay Active in Nashville
Mar 10, 2023

Does Medicare Cover Scleral Lenses?
Dec 5, 2022
Does Medicare Cover an FMT?
Dec 2, 2022

Do All Hospitals Accept Medicare Advantage Plans?
Apr 11, 2023
Can I Use Medicare Part D at Any Pharmacy?
Aug 28, 2023

How Do Medigap Premiums Vary?
Apr 12, 2023

Is Vitrectomy Surgery Covered by Medicare?
Dec 2, 2022

Does Medicare Cover TENS Units?
Nov 23, 2022

Does Medicare Cover SIBO Testing?
Dec 1, 2022

Do Medicare Supplement Plans Cover Dental and Vision?
Dec 8, 2022

Will Medicare Cover Dental Implants?
Jun 2, 2022

Does Medicare Have Limitations on Hospital Stays?
Mar 15, 2024
More of our articles
13 Best Ways for Seniors to Stay Active in Columbus
13 Best Ways for Seniors to Stay Active in Jacksonville
13 Best Ways for Seniors to Stay Active in Phoenix
20 Questions to Ask Your Medicare Agent
2025 Medicare Price Changes
Can I Change Medicare Advantage Plans Any Time? | Medicare Plans
Can I Choose Marketplace Coverage Instead of Medicare?
Can I Laminate My Medicare Card?
Comparing All Medigap Plans | Chart Updated for 2025
Do I Need to Renew My Medicare?
Does Medicare Cover a Spinal Cord Stimulator?
Does Medicare Cover Abortion Services?
Does Medicare Cover Bladder Sling Surgery?
Does Medicare Cover Boniva?
Does Medicare Cover Disposable Underwear?
Does Medicare Cover Driving Evaluations?
Does Medicare Cover Exercise Physiology?
Does Medicare Cover Flu Shots?
Does Medicare Cover Hearing Aids?
Does Medicare cover Hyoscyamine?
Does Medicare Cover Hypnotherapy?
Does Medicare Cover Ilumya?
Does Medicare Cover Incontinence Supplies?
Does Medicare Cover Inspire for Sleep Apnea?
Does Medicare Cover Jakafi?
Does Medicare Cover Krystexxa?
Does Medicare Cover Kyphoplasty?
Does Medicare Cover Mental Health?
Does Medicare Cover Nuedexta?
Does Medicare Cover Ozempic?
Does Medicare Cover Penile Implant Surgery?
Does Medicare Cover Robotic Surgery?
Does Medicare Cover Urodynamic Testing?
Does Medicare Cover Wart Removal?
Does Medicare Cover Zilretta?
Does Medicare Pay for Bunion Surgery?
Does Medicare pay for Opdivo?
Does Medicare Pay for Varicose Vein Treatment?
Does Medicare Require a Referral for Audiology Exams?
Fair Square Bulletin: We're Revolutionizing Medicare
Fair Square Client Newsletter: AEP Edition
How Can I Get a Replacement Medicare Card?
How Do Medicare Agents Get Paid?
How Does Medicare Cover Colonoscopies?
How Does the End of the COVID-19 Public Health Emergency Affect Your Medicare?
How is Medicare Changing in 2025?
How Much Does a Pacemaker Cost with Medicare?
How Much Does Open Heart Surgery Cost with Medicare?
How Much Does Xeljanz Cost with Medicare?
How to Become a Medicare Agent
How to Choose a Medigap Plan
How Your Employer Insurance and Medicare Work Together
Is Displacement Affecting Your Medicare Coverage?
Is Emsella Covered by Medicare?
Is Fair Square Medicare Legitimate?
Last Day to Change Your Medicare Part D Plan
Medicare Advantage Plans for Disabled People Under 65
Medicare Deductibles Resetting in 2025
Medicare Savings Programs in Kansas
Medicare Supplement Plans for Low-Income Seniors
Medigap Plan N vs. Plan G — Which One Fits You in 2025?
Medigap vs. Medicare Advantage
Should You Work With A Remote Medicare Agent?
Top 10 Physical Therapy Clinics in San Diego
What If I Don't Like My Plan?
What is a Medicare Beneficiary Ombudsman?
What Is a Medicare Supplement SELECT Plan?
What Is Medical Underwriting for Medigap?
What Is the Medicare Birthday Rule in Nevada?
What To Do If Your Medicare Advantage Plan Is Discontinued
What's the Deal with Flex Cards?
Why Is Medicare So Confusing?
Get the Fair Square Bulletin
Medicare savings tips, helpful guides, and more.
Virgil Insurance Agency, LLC (DBA Fair Square Medicare) and www.fairsquaremedicare.com are privately owned and operated by Help Button Inc. Medicare supplement insurance plans are not connected with or endorsed by the U.S. government or the federal Medicare program. This is a solicitation of insurance. A licensed agent/producer may contact you. Medicare Supplement insurance is available to those age 65 and older enrolled in Medicare Parts A and B and, in some states, to those under age 65 eligible for Medicare due to disability or End-Stage Renal disease. Virgil Insurance Agency is a licensed and certified representative of Medicare Advantage HMO, HMO SNP, PPO, PPO SNP and PFFS organizations and stand-alone PDP prescription drug plans. Each of the organizations we represent has a Medicare contract. Enrollment in any plan depends on contract renewal. The plans we represent do not discriminate on the basis of race, color, national origin, age, disability, or sex. Plan availability varies by region and state. For a complete list of available plans please contact 1-800-MEDICARE (TTY users should call 1-877-486-2048), 24 hours a day/7 days a week or consult www.medicare.gov. © 2026 Help Button Inc
We do not offer every plan available in your area. Any information we provide is limited to those plans we do offer in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options.
MULTIPLAN_FairSquareMedicare_01062022_M
Fair Square Medicare


